GluteGuard Module 2: Accidental Gluten Ingestion
A gluten free diet remains the only treatment available for coeliac disease and other gluten-related disorders. Management of these conditions and their symptoms relies entirely on accurate dietary adherence1.
While adherence typically improves with experience, individuals don’t always have complete control over how their food is prepared, which often leads to accidental gluten ingestion.
Accidental gluten ingestion
Accidental gluten ingestion is the unintentional consumption of gluten despite efforts to ensure a meal or food item is gluten free.
Often described as being “glutened”, this experience is not the result of carelessness or deliberate choice. Instead, it reflects the reality of eating food prepared by others, where there is limited control over ingredients and preparation methods.
Gluten free foods are often prepared or served in environments where gluten is also present, making it difficult to entirely eliminate the risk of exposure.
Several studies suggest that most individuals on a strict gluten free diet regularly consume enough gluten to trigger symptoms and other unwanted effects2.
Common causes include:

Shared environments: Using the same utensils, equipment, or surfaces for glutencontaining and gluten free foods during manufacturing, storage, preparation, or service.

Unclear labelling: Mislabelled foods or ingredients, or product labels that are difficult to read or inconsistently formatted.

Human error: Mix ups, unfamiliarity with gluten sources, misreading ingredient lists, distractions, or simply forgetting.

Misunderstandings: Miscommunication in busy environments, differing interpretations of gluten free requirements, or cultural and language barriers.
Where does accidental gluten ingestion happen?
Unintentional gluten exposure typically occurs in situations where food is prepared outside of one’s control, such as:
The impact of accidental gluten ingestion
For individuals following a gluten free diet, accidental gluten ingestion can be an ongoing source of stress. Even as little as 10mg of gluten (a few breadcrumbs) can trigger symptoms in the most sensitive individuals3. Symptoms vary in type, timing, and severity, and may disrupt daily routines or important plans.
The risk of being “glutened” can lead to increased anxiety around gluten free dining, where control over food preparation is limited4. This anxiety can manifest as food-related hypervigilance and social withdrawal4,5. While these behaviours are intended to reduce risk, they can ultimately contribute to a lower quality of life4,5.


How GluteGuard offers protection
GluteGuard is the world’s only clinically proven protection from symptoms of accidental gluten ingestion6,7.
GluteGuard is recommended to be taken 5–15 minutes before eating, whenever there’s a risk of being “glutened”. This way, GluteGuard’s enzymes are ready to act in the small intestine, helping to break down gluten peptides before they interact with the intestinal lining and trigger symptoms.
This added protection helps individuals approach gluten free dining, social occasions, and travel with greater confidence.
Want a chance to win $1,000?
Simply answer the quiz question correctly and you’ll be in the draw to win!
References
1. Sapone A, et al. Spectrum of gluten-related disorders: consensus on new nomenclature and classification. BMC Med. 2012 Feb 7;10(1):13.
2. R Wieser H, et al. Challenges of monitoring the gluten-free diet adherence in the management and follow-up of patients with celiac disease. Nutrients. 2021 Jun 30;13(7):227.
3. Catassi C, et al. A prospective, double-blind, placebo-controlled trial to establish a safe gluten threshold for patients with celiac disease. Am J Clin Nutr. 2007 Jan 1;85(1):160-166.
4. Lee AR, et al. Factors Associated with Maladaptive Eating Behaviors, Social Anxiety, and Quality of Life in Adults with Celiac Disease. Nutrients. 2021; 13(12):4494.
5. Wolf RL, et al. Hypervigilance to a gluten-free diet and decreased quality of life in teenagers and adults with celiac disease. Dig Dis Sci. 2018 Jun;63(6):1438-48.
6. Cornell HJ, et al. The effect of enzyme supplementation on symptoms and duodenal histology in celiac patients. Int J Celiac Dis. 2016;4:40-47.
7. Żebrowska A, et al. The effect of enzyme therapy on skin symptoms and immune responses in patients with dermatitis herpetiformis. Int J Celiac Dis. 2014;2(2):58-63.
A gluten free diet remains the only treatment available for coeliac disease and other gluten-related disorders. Management of these conditions and their symptoms relies entirely on accurate dietary adherence1.
While adherence typically improves with experience, individuals don’t always have complete control over how their food is prepared, which often leads to accidental gluten ingestion.
Accidental gluten ingestion
Accidental gluten ingestion is the unintentional consumption of gluten despite efforts to ensure a meal or food item is gluten free.
Often described as being “glutened”, this experience is not the result of carelessness or deliberate choice. Instead, it reflects the reality of eating food prepared by others, where there is limited control over ingredients and preparation methods.
Gluten free foods are often prepared or served in environments where gluten is also present, making it difficult to entirely eliminate the risk of exposure.
Several studies suggest that most individuals on a strict gluten free diet regularly consume enough gluten to trigger symptoms and other unwanted effects2.
Common causes include:

Shared environments: Using the same utensils, equipment, or surfaces for glutencontaining and gluten free foods during manufacturing, storage, preparation, or service.

Unclear labelling: Mislabelled foods or ingredients, or product labels that are difficult to read or inconsistently formatted.

Human error: Mix ups, unfamiliarity with gluten sources, misreading ingredient lists, distractions, or simply forgetting.

Misunderstandings: Miscommunication in busy environments, differing interpretations of gluten free requirements, or cultural and language barriers.
Where does accidental gluten ingestion happen?
Unintentional gluten exposure typically occurs in situations where food is prepared outside of one’s control, such as:
The impact of accidental gluten ingestion
For individuals following a gluten free diet, accidental gluten ingestion can be an ongoing source of stress. Even as little as 10mg of gluten (a few breadcrumbs) can trigger symptoms in the most sensitive individuals3. Symptoms vary in type, timing, and severity, and may disrupt daily routines or important plans.
The risk of being “glutened” can lead to increased anxiety around gluten free dining, where control over food preparation is limited4. This anxiety can manifest as food-related hypervigilance and social withdrawal4,5. While these behaviours are intended to reduce risk, they can ultimately contribute to a lower quality of life4,5.


How GluteGuard offers protection
GluteGuard is the world’s only clinically proven protection from symptoms of accidental gluten ingestion6,7.
GluteGuard is recommended to be taken 5–15 minutes before eating, whenever there’s a risk of being “glutened”. This way, GluteGuard’s enzymes are ready to act in the small intestine, helping to break down gluten peptides before they interact with the intestinal lining and trigger symptoms.
This added protection helps individuals approach gluten free dining, social occasions, and travel with greater confidence.
How GluteGuard offers protection
GluteGuard is the world’s only clinically proven protection from symptoms of accidental gluten ingestion6,7.
GluteGuard is recommended to be taken 5–15 minutes before eating, whenever there’s a risk of being “glutened”. This way, GluteGuard’s enzymes are ready to act in the small intestine, helping to break down gluten peptides before they interact with the intestinal lining and trigger symptoms.
This added protection helps individuals approach gluten free dining, social occasions, and travel with greater confidence.

Want a chance to win $1,000?
Simply answer the quiz question correctly and you’ll be in the draw to win!
Want a chance to win $1,000?
Simply answer the quiz question correctly and you’ll be in the draw to win!
References
1. Sapone A, et al. Spectrum of gluten-related disorders: consensus on new nomenclature and classification. BMC Med. 2012 Feb 7;10(1):13.
2. R Wieser H, et al. Challenges of monitoring the gluten-free diet adherence in the management and follow-up of patients with celiac disease. Nutrients. 2021 Jun 30;13(7):227.
3. Catassi C, et al. A prospective, double-blind, placebo-controlled trial to establish a safe gluten threshold for patients with celiac disease. Am J Clin Nutr. 2007 Jan 1;85(1):160-166.
4. Lee AR, et al. Factors Associated with Maladaptive Eating Behaviors, Social Anxiety, and Quality of Life in Adults with Celiac Disease. Nutrients. 2021; 13(12):4494.
5. Wolf RL, et al. Hypervigilance to a gluten-free diet and decreased quality of life in teenagers and adults with celiac disease. Dig Dis Sci. 2018 Jun;63(6):1438-48.
6. Cornell HJ, et al. The effect of enzyme supplementation on symptoms and duodenal histology in celiac patients. Int J Celiac Dis. 2016;4:40-47.
7. Żebrowska A, et al. The effect of enzyme therapy on skin symptoms and immune responses in patients with dermatitis herpetiformis. Int J Celiac Dis. 2014;2(2):58-63.
GluteGuard Module 1: Gluten Digestion
What is gluten?
Gluten is a protein found in wheat, barley, and rye, including varieties and derivative species of these grains, such as spelt, triticale, and durum1.
Gluten isn’t a single protein, but rather a combination of two main types of proteins: gliadin and glutenin1.
When combined with water, these proteins bond together to form the stretchy, elastic network that gives bread, pasta, and other baked goods their characteristic texture2.
Gluten digestion
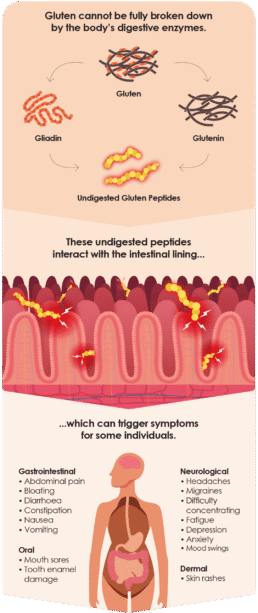
When gluten is consumed, the body’s digestive enzymes are unable to fully break down gliadin and glutenin, leaving behind partially digested proteins called peptides1.
In the small intestine, these undigested peptides can interact with cells in the intestinal lining or cross through the gut barrier, causing problems for susceptible individuals3.
Who is gluten a problem for?
For most people, these undigested gluten peptides continue through the digestive system without issue.
However, in individuals with gluten-related disorders, they can trigger a variety of intestinal or extraintestinal symptoms when they interact with the lining of the small intestine4.
In coeliac disease, these peptides also trigger immune activation and inflammation that lead to intestinal damage1.
Treatment for gluten-related disorders
A gluten free diet remains the only treatment available for gluten-related disorders such as coeliac disease, dermatitis herpetiformis, and non-coeliac wheat/gluten sensitivity.
However, even with careful dietary adherence, accidental gluten ingestion is common – particularly when eating outside the home, where meal preparation is difficult to control5.
How GluteGuard helps
GluteGuard supports the maintenance of a gluten free diet by protecting against symptoms of accidental gluten ingestion6, 7.
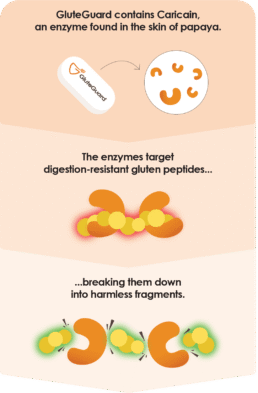
It contains Caricain, a unique enzyme found in the skin of unripe papaya, which is able to break down the digestion-resistant gluten peptides known to trigger symptoms in people with gluten-related disorders8.
Taken before a meal as a pre-emptive measure, GluteGuard helps to break these peptides into smaller, harmless fragments before they can interact with the intestinal lining and trigger symptoms.
In this way, GluteGuard offers protection against symptoms of accidental gluten ingestion and peace of mind when meals are prepared by others.
What is gluten?
Gluten is a protein found in wheat, barley, and rye, including varieties and derivative species of these grains, such as spelt, triticale, and durum1.
Gluten isn’t a single protein, but rather a combination of two main types of proteins: gliadin and glutenin1.
When combined with water, these proteins bond together to form the stretchy, elastic network that gives bread, pasta, and other baked goods their characteristic texture2.
Gluten digestion
When gluten is consumed, the body’s digestive enzymes are unable to fully break down gliadin and glutenin, leaving behind partially digested proteins called peptides1.
In the small intestine, these undigested peptides can interact with cells in the intestinal lining or cross through the gut barrier, causing problems for susceptible individuals3.
Who is gluten a problem for?
For most people, these undigested gluten peptides continue through the digestive system without issue.
However, in individuals with gluten-related disorders, they can trigger a variety of intestinal or extraintestinal symptoms when they interact with the lining of the small intestine4.
In coeliac disease, these peptides also trigger immune activation and inflammation that lead to intestinal damage1.

Treatment for gluten-related disorders
A gluten free diet remains the only treatment available for gluten-related disorders such as coeliac disease, dermatitis herpetiformis, and non-coeliac wheat/gluten sensitivity.
However, even with careful dietary adherence, accidental gluten ingestion is common – particularly when eating outside the home, where meal preparation is difficult to control5.
How GluteGuard helps
GluteGuard supports the maintenance of a gluten free diet by protecting against symptoms of accidental gluten ingestion6, 7.
It contains Caricain, a unique enzyme found in the skin of unripe papaya, which is able to break down the digestion-resistant gluten peptides known to trigger symptoms in people with gluten-related disorders8.
Taken before a meal as a pre-emptive measure, GluteGuard helps to break these peptides into smaller, harmless fragments before they can interact with the intestinal lining and trigger symptoms.
In this way, GluteGuard offers protection against symptoms of accidental gluten ingestion and peace of mind when meals are prepared by others.
References
1. Biesiekierski, JR. What is gluten?. J Gastroenterol Hepatol, 2017;32:78–81.
2. Aljada B, Zohni A, El-Matary W. The gluten-free diet for celiac disease and beyond. Nutrients. 2021 Nov 9;13(11):3993.
3. Cebolla Á, Moreno MD, Coto L, et al. Gluten immunogenic peptides as standard for the evaluation of potential harmful prolamin content in food and human specimen. Nutrients. 2018 Dec 5;10(12):1927.
4. Sapone A, Bai JC, Ciacci C, et al. Spectrum of gluten-related disorders: consensus on new nomenclature and classification. BMC Med. 2012 Feb 7;10(1):13.
5. Silvester JA, Graff LA, Rigaux L, et al. Symptomatic suspected gluten exposure is common among patients with coeliac disease on a gluten-free diet. Aliment Pharmacol Ther. 2016 Sep;44(6):612-619.
6. Cornell HJ, Czyzewska A, Macrae FA, et al. The effect of enzyme supplementation on symptoms and duodenal histology in celiac patients. Int J Celiac Dis. 2016;4:40-47.
7. Żebrowska A, Cornell HJ, Macrae FA, et al. The effect of enzyme therapy on skin symptoms and immune responses in patients with dermatitis herpetiformis. Int J Celiac Dis. 2014;2(2):58-63.
8. Tanner GJ. Relative rates of gluten digestion by nine commercial dietary digestive supplements. Front Nutr. 2021 Dec 7;8:784850.
GluteGuard Quick Guide
Who GluteGuard helps
GluteGuard helps to support the maintenance of a gluten free diet for individuals living with gluten related disorders, such as:
- Coeliac disease
- Non-coeliac wheat/gluten sensitivity
- Dermatitis herpetiformis
While a strict gluten free diet remains the only treatment available for gluten-related disorders, avoiding gluten entirely can be challenging, and accidental gluten ingestion is a common occurrence.
How GluteGuard helps
GluteGuard breaks down gluten before it can cause symptoms.
- Taken before a meal, GluteGuard offers protection by breaking down hidden gluten before it interacts with the intestinal lining and triggers symptoms.
- Contains Caricain, a naturally-derived enzyme that targets the specific gluten peptides responsible for symptoms of gluten ingestion.
- Clinically trialled in individuals with coeliac disease1 and dermatitis herpetiformis2.

When to use GluteGuard
GluteGuard is recommended for use alongside a gluten free diet, in situations where there’s a risk of accidental gluten ingestion, such as:
Key things to remember
For those medically required to avoid gluten
GluteGuard is suitable for individuals with coeliac disease and other medically diagnosed gluten sensitivities when used alongside a gluten free diet.
Enzyme-based action
GluteGuard’s enzyme acts locally in the digestive tract and is not known to build up or interact with the body. Excess enzymes simply pass through the digestive system and are naturally excreted.
Taking before a meal
To help protect against symptoms of accidental gluten ingestion, GluteGuard’s enzymes must be present in the small intestine before food arrives. This ensures they’re ready to help break down any hidden gluten before it interacts with the intestinal lining and triggers symptoms.
Use on a regular basis
GluteGuard’s active ingredient is naturally derived from papaya and is suitable for regular use. With a maximum daily dose of 4 tablets, it can be taken before each meal in situations of ongoing risk, such as when travelling.
Product information
GluteGuard helps protect those with medically diagnosed gluten sensitivity from symptoms of accidental gluten ingestion.
ACTIVE INGREDIENT
Each enteric-coated tablet contains:
Carica papaya fruit oleoresin dry (Caricain) 300mg
DOSAGE
Adults: Take 1 whole tablet orally immediately before a meal, or as recommended by a healthcare professional.
Do not crush, break or chew.
Maximum daily dose should not exceed 4 tablets unless otherwise recommended by a healthcare professional.
Recommended for adults aged 18 years and older.
WARNINGS
- Do not use if allergic to papaya (paw paw) or natural rubber latex.
- Do not use if pregnant or breastfeeding.
- Do not use if taking blood-thinning medication (warfarin).
- Contains sulphites.
If symptoms persist, worsen or episodes become more frequent, refer on to a medical practitioner.
TO BE USED IN CONJUNCTION WITH A GLUTEN FREE DIET
References
1. Cornell HJ, Czyzewska A, Macrae FA, et al. The effect of enzyme supplementation on symptoms and duodenal histology in celiac patients. Int J Celiac Dis. 2016;4:40-47.
2. Żebrowska A, Cornell HJ, Macrae FA, et al. The effect of enzyme therapy on skin symptoms and immune responses in patients with dermatitis herpetiformis. Int J Celiac Dis. 2014;2(2):58-63.